COVID LOCAL
A Frontline Guide for Local Decision-Makers
The COVID-19 pandemic has caused significant disruptions to cities and local communities globally. Given these challenges, in March 2020 we developed this guide to provide a decision framework for local leaders to think through what needs to be done to help reduce the impact of the outbreak, both by reducing spread and decreasing the number of cases, but also in responding and supporting communities effectively.
Metrics for Phased Reopening
Developed in Spring 2020 to help local level leaders plan for phased reopening as well as when to reinstitute control measures
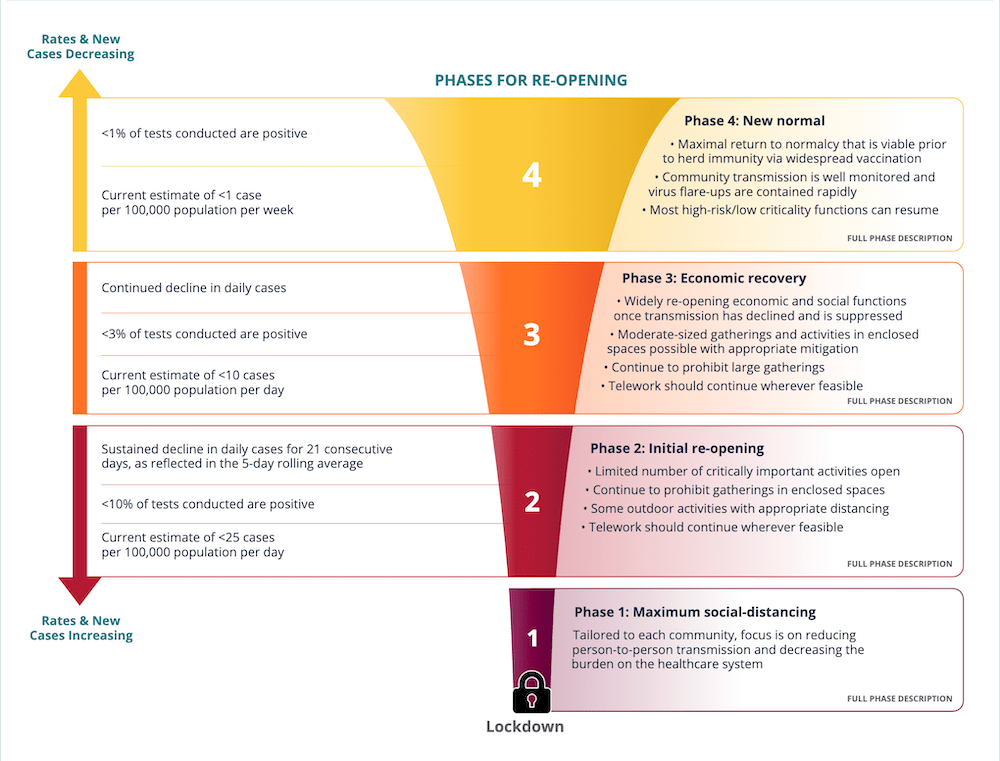 Go to Metrics
Go to MetricsBLOG
Notes from the field
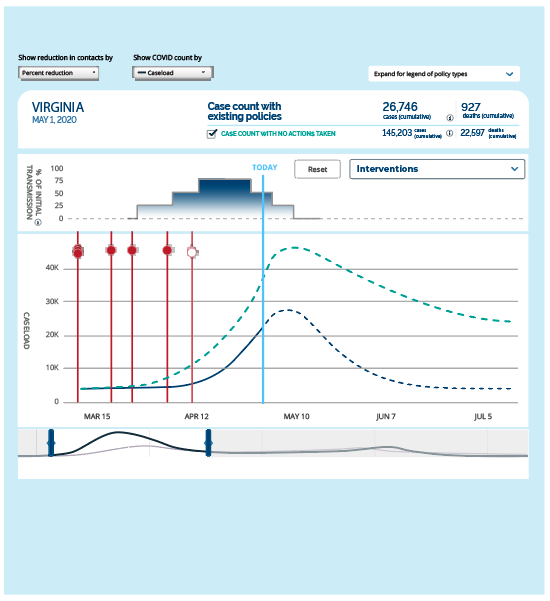
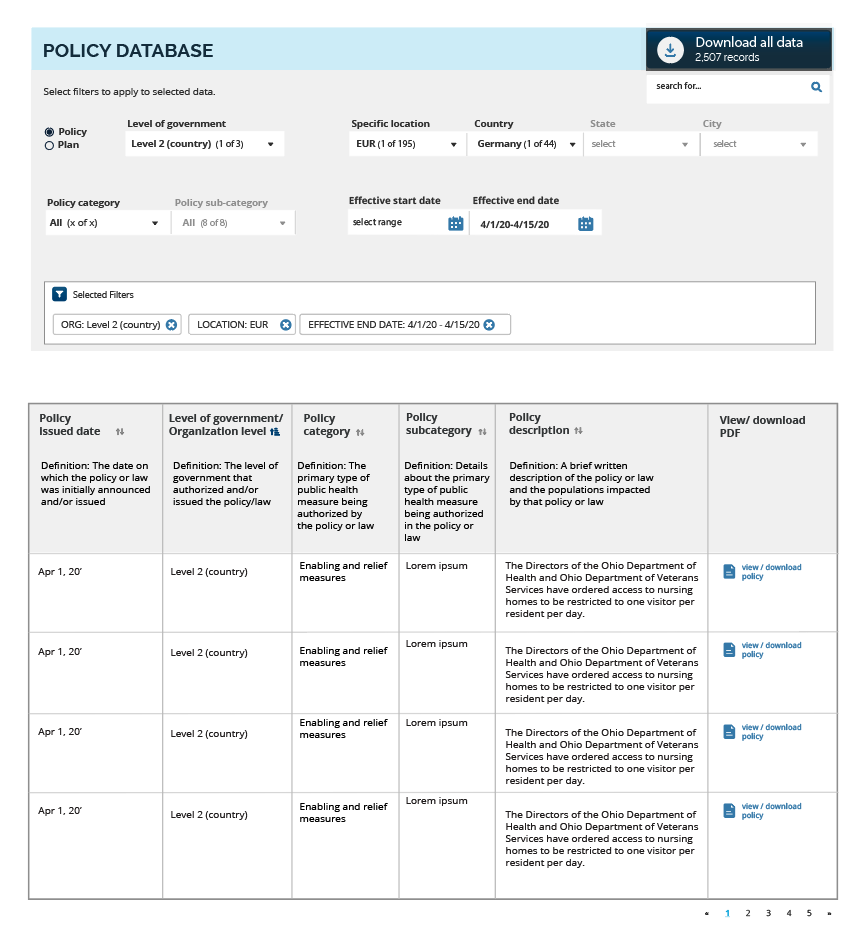
COVID AMP Database and Modeling Tool: Assess How Well Your Pandemic Policies Have Worked
2020-08-27
Needing to understand what policies are effective? Struggling with knowing how to flatten the curve in your community? The team behind COVID-Local.org launched a policy modeling tool and database of tens of thousands of COVID-19 response policies and plans enacted across the U.S. and countries around the world. COVID... read more
LEARN
Ask The Experts
A brief list of topics, relevant resources, and options to contact leading experts for additional information.
Go to Ask The Experts